 The 2016 Infusion Therapy Standards of Practice have already generated questions about one hot issue – should short peripheral catheters be routinely aspirated for a blood return to assess their patency? For the first time, this document includes a definition of “blood return” in the glossary, stating this is a component of VAD patency assessment and that the blood should be the color and consistency of whole blood. Blood return from peripheral catheters is included in standards on documentation, flushing and locking, VAD assessment, VAD removal, infiltration and extravasation, and antineoplastic agents. Many old nursing references state that reliance on blood return is not adequate to determine if the catheter is infiltrating fluid. The nurse can not rely exclusively on the presence of absence of a blood return before using the peripheral catheter. There could easily be a second puncture in the posterior vein wall and still get a blood return OR there could be a small catheter occluded by aspiration technique. For these reasons, the assessment must also include observing the appearance of the site, including comparison to the opposite extremity; palpating for change in temperature or induration; and patient complaints about the site. Other reasons for a lack of blood return could be damage to the endothelial vein lining producing edema or small thrombi that occlude the back flow of blood. Fluid may not be escaping from the vein – yet. But this damage can lead to infiltration or extravasation and continued use will only exacerbate the current complication. Complications are seen more frequently when venous sites in the hand, wrist, and antecubital fossa are used. The 2016 Standards now call for obtaining a blood sample from a peripheral catheter during the dwell time instead of during the insertion procedure. Studies are showing that this is a successful practice. If the peripheral catheter will yield a blood sample, it can easily produce a blood return for patency assessment. As I mentioned, technique can be the cause of failure to obtain a blood return. First and foremost, use a slow and gentle technique to aspirate from the catheter. Pulling hard and fast on the syringe plunger can pull the vein wall over the catheter lumen. Next, change to a smaller syringe as aspiration with a smaller syringe produces less pressure and better results. That is opposite from what happens with injection where a larger syringe is recommended. Finally, put a tourniquet on the arm above the catheter tip to see if there is a blood return. If all of these techniques fail to produce a blood return, do NOT use the catheter. Everyone can think of many examples of complications associated with vascular access devices and infusion therapy. Textbooks and all types of journal publications provide much information about the signs and symptoms, prevention, and management of these events - always with the goal of prevention.
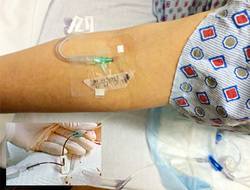
What about those adverse events that are not found in the published literature? Do they actually happen? If a study or case report about a specific complication can not be found in the published literature should we dismiss the idea that it could happen? A primary example is venous air embolism (VAE) following the removal of a PICC. The catheter is slowly withdrawn from the vein and pressure is applied to stop any bleeding. Do we need to use the same precautions to prevent VAE with a PICC removal as we use with a subclavian or jugular insertion site? After searching extensively through the published literature in the English language, there are no publications that have documented VAE with PICC removal. There are a few reports of VAE with PICCs occurring due to attaching an unprimed administration set but none occurring during PICC removal. Based on anatomy and physiology, we know that a skin-to-vein tract can develop especially with lengthy catheter dwell times. Also, a fibrin sheath frequently covers the entire length of catheter and could remain intact inside the vein when the catheter is removed. The 2016 Infusion Therapy Standards of Practice includes this information and advises to use methods to prevent VAE for all central vascular access devices (CVAD). In my opinion, we must use our knowledge of vascular anatomy and the physiology of blood flow, merged with our critical thinking skills based on patient assessment. Armed with this information, our professional responsibility is to apply the safest methods possible to prevent such events. Additionally, if an unreported event occurs in your facility, please share your experience by publishing your case report. No publications on a complication, yet anatomical and physiological evidence supports the possibility indicates the need to apply the usual precautions in this example. What is your opinion? |
Author: Lynn HadawayLynn Hadaway is an international thought leader in infusion therapy and vascular access, having been in this practice for more than 40 years. Her experience comes from hospital-based infusion teams, device manufacturers, and continuing education services. Her journal and textbook publications are extensive. She also maintains board certification in infusion nursing (CRNI) and nursing professional development (RN-BC). Categories
Archives
May 2019
|
Copyright © 2020 Lynn Hadaway Associates, Inc. | P.O. Box 10, Milner, GA 30257 | 770-358-7861


 RSS Feed
RSS Feed