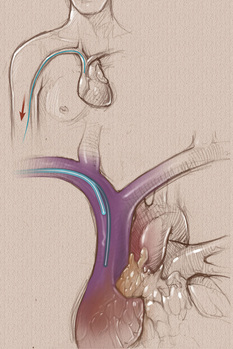
 Have you ever had a patient complain of strange heart flutters, palpitations, or even chest pain when a PICC is indwelling? What can be done and who should do it? After PICC insertion, the tip is not stationary. Inserters make every attempt to get the catheter tip at the cavoatrial junction, however arm movement can and often does alter this location. For PICCs, this will usually means the tip moves inward, into the right atrium. This can cause the cardiac flutter feeling or your patient may complain of feeling a fast or irregular heartbeat. Retraction of the PICC by a very short distance may be needed to relieve these symptoms. Who should be doing this catheter repositioning – the nurse inserting the PICC or the primary care nurse? Legally speaking, this procedure may be within the legal scope of practice for both registered nurses, BUT a policy from your organization is necessary to direct who can actually perform this procedure. There are several decisions to be made before any central VAD is repositioned. Where was the original tip documented – precisely? How was this tip location confirmed – chest xray or ECG? According to the 2016 Infusion Therapy Standards of Practice, the tip of any CVAD can be anywhere from the lower third of the superior vena cava and extend into the right atrium by 2 cm. If the original placement was at the cavoatrial junction, arm movement may have taken the tip more than 2 cm into the right atrium and this indicates the need for retraction if the patient has any cardiac complaints. A chest xray may be necessary before this retraction to provide more precise information on the safe length that should be retracted. The adult superior vena cava is usually about 7 cm long. CVAD tips located in the mid to upper SVC are more prone to complications such as tip migration into the jugular vein and vein thrombosis. Retraction without a precise measurement could result in a suboptimal tip location which increases patient risk. The policy and procedure written and approved by each facility must address which nurse will be doing this procedure. It is my professional opinion that this catheter manipulation should only be performed by the nurse with documented competency with PICC insertion. It should not be performed by the primary care nurse, or anyone without the detailed knowledge and skills for PICC insertion. Retraction itself is not a difficult task, but there are many aspects of patient assessment, critical thinking and decision-making required. The facility policy should also require documented competency to perform this procedure, especially if the responsibility is given to the primary care nurse. Two standards of practice address this issue. Please read Standard 53 CVAD Malposition and don’t forget the Section Standards on page 103 as they apply to all standards in this section. The second standard is #5 Competency Assessment and Validation. You should also check with your state board of nursing for any specific statements they may have about PICC insertion and management.  The 2016 Infusion Therapy Standards of Practice used many “action” verbs to start the Practice Criteria statements. A quick look through this document shows “assess”, “use”, “perform”, “determine”, “choose”, “select”, and many others. But this examination of the document also reveals another word in common use – “consider”. Is there a difference in these verbs? If so, what is that difference? This is an evidence-based document, meaning the committee searched the published literature and carefully evaluated all evidence. As indicated in the rating scale found on page S10 of the document, there is a hierarchy of these studies based on the study design. There are several ways to evaluate this found evidence. Multiple studies with good research design and study processes that produced consistent results received a high rating, usually a grade of I or II. These statements are the ones that begin with the strong action verbs. As you would imagine, this high level of evidence was not always found. Sometimes, the study design and process was good, but the outcome of several studies may be inconclusive or conflicting. This indicated the need for a lower rating. These practice criteria statements begin with “consider” and require a closer examination for your practice. These statements go on to provide specific criteria that should be contemplated. You may be using these statements to make decisions about a specific patient situation or to write facility policies and procedures. These “consider” statements will require more critical thinking on your part. You may need to think about all aspects of care for a specific patient or the needs of a larger patient population. The expertise or skill level of your staff, and the staffing mix such as RN versus LPN/LVN versus unlicensed assistants may need to be deliberated. Additionally, you may reach a different practice decision based on the venue of care, considering the differences between hospitals, skilled nursing facilities, an ambulatory clinic, or the home. The bottom line is that there continues to be many aspects of practice without concrete answers to every question. You may need to look up the references provided to obtain more details to guide your decision. This process requires a high level of critical thinking skills and good nursing judgment. The body of evidence is improving, however we will never have all the needed answers, so critical thinking is a necessary skill to develop. Pay attention to the action verbs and the rankings of evidence to reach the most appropriate decisions. 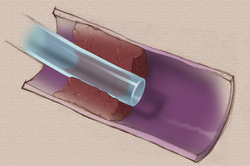 Catheter associated vein thrombosis can be a significant problem with some central vascular access devices, especially PICCs. The question about immediate removal is always first and foremost on the minds of most nurses. A color duplex ultrasound study can be used to show extensive thrombosis in either vein where the catheter lies. It may also demonstrate no blood flow in those same veins. Where should the removal procedure take place – in the patient’s room, a treatment room, or in Radiology under fluoroscopy? Who should do the removal procedure – primary care nurse, nurse inserting the PICC, primary physician, radiologists? First, don’t be too quick to advocate for removal. Before you consider where and by whom the catheter will be removed, there are some other questions that should be addressed. Your answers to these questions may indicate that the catheter should be left in place. Does this patient continue to require a central venous catheter after considering the remaining length of infusion therapy and its characteristics? Is it possible that the infusion therapy is near the end and it may be discontinued or changed to another route? This will require reading the progress notes of the licensed independent practitioner(s) (LIP) and discussing the situation with them. Before you initiate this discussion, gather some additional information. If fluids are infusing, what is the patient’s ability to eat and drink? Are vital signs normal and stable? What medications are being given? What is the anticipated length of time remaining on this plan of care? If only a few more days, a change to oral medication may be possible. Next assess where the catheter is located and how well it is functioning. Is the catheter tip in the recommended position in the lower SVC near or at the cavoatrial junction? Is the catheter functioning with a good blood return and no resistance to fluid flow through the catheter? If the catheter is correctly positioned and there is a blood return and there is no resistance to flushing or fluid infusion, this strongly favors leaving the catheter in place. Next consider all systemic signs and symptoms the patient may have. Are there any signs or symptoms, concern or thoughts of bloodstream infection being present? If yes, this could mean an infected thrombus and will usually mean catheter removal. Is the patient complaining of pain or any type of excessive discomfort in the arm, neck, shoulder, or chest, especially on the ipsilateral side of the catheter? These complaints may mean it is more than the patient is able to tolerate, however treatment may help to improve those complaints. Immediate removal when there is a need for another CVAD insertion may not be the best option. The next catheter could easily produce a similar event on the other side, so the goal is usually to leave it in place. The patient should be treated for DVT with systemic anticoagulation for as long as the CVAD is needed and for 3 months after it is removed. Information about this is found in two INS Standards - Standard 52 CVAD Associated Thrombosis and Standard 44 VAD Removal. The medical references are two evidence based guidelines. You might want to find these and share with colleagues and appropriate committees in your facility. Both of these publications can be downloaded free of charge. Click below to get the full text. Kearon, C., Akl, E. A., Comerota, A. J., Prandoni, P., Bounameaux, H., Goldhaber, S. Z., . . . Dentali, F. (2012). Antithrombotic therapy for VTE disease: antithrombotic therapy and prevention of thrombosis: American College of Chest Physicians evidence-based clinical practice guidelines. CHEST Journal, 141(2_suppl), e419S-e494S. http://www.ncbi.nlm.nih.gov/pmc/articles/PMC3278049/pdf/112301.pdf Debourdeau, P., Farge, D., Beckers, M., Baglin, C., Bauersachs, R. M., Brenner, B., . . . Bounameaux, H. (2013). International clinical practice guidelines for the treatment and prophylaxis of thrombosis associated with central venous catheters in patients with cancer. J Thromb Haemost, 11(1), 71-80. doi:10.1111/jth.12071 http://onlinelibrary.wiley.com/doi/10.1111/jth.12071/epdf |
Author: Lynn HadawayLynn Hadaway is an international thought leader in infusion therapy and vascular access, having been in this practice for more than 40 years. Her experience comes from hospital-based infusion teams, device manufacturers, and continuing education services. Her journal and textbook publications are extensive. She also maintains board certification in infusion nursing (CRNI) and nursing professional development (RN-BC). Categories
Archives
May 2019
|
Copyright © 2020 Lynn Hadaway Associates, Inc. | P.O. Box 10, Milner, GA 30257 | 770-358-7861


 RSS Feed
RSS Feed