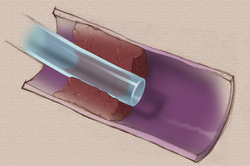
 Catheter associated vein thrombosis can be a significant problem with some central vascular access devices, especially PICCs. The question about immediate removal is always first and foremost on the minds of most nurses. A color duplex ultrasound study can be used to show extensive thrombosis in either vein where the catheter lies. It may also demonstrate no blood flow in those same veins. Where should the removal procedure take place – in the patient’s room, a treatment room, or in Radiology under fluoroscopy? Who should do the removal procedure – primary care nurse, nurse inserting the PICC, primary physician, radiologists? First, don’t be too quick to advocate for removal. Before you consider where and by whom the catheter will be removed, there are some other questions that should be addressed. Your answers to these questions may indicate that the catheter should be left in place. Does this patient continue to require a central venous catheter after considering the remaining length of infusion therapy and its characteristics? Is it possible that the infusion therapy is near the end and it may be discontinued or changed to another route? This will require reading the progress notes of the licensed independent practitioner(s) (LIP) and discussing the situation with them. Before you initiate this discussion, gather some additional information. If fluids are infusing, what is the patient’s ability to eat and drink? Are vital signs normal and stable? What medications are being given? What is the anticipated length of time remaining on this plan of care? If only a few more days, a change to oral medication may be possible. Next assess where the catheter is located and how well it is functioning. Is the catheter tip in the recommended position in the lower SVC near or at the cavoatrial junction? Is the catheter functioning with a good blood return and no resistance to fluid flow through the catheter? If the catheter is correctly positioned and there is a blood return and there is no resistance to flushing or fluid infusion, this strongly favors leaving the catheter in place. Next consider all systemic signs and symptoms the patient may have. Are there any signs or symptoms, concern or thoughts of bloodstream infection being present? If yes, this could mean an infected thrombus and will usually mean catheter removal. Is the patient complaining of pain or any type of excessive discomfort in the arm, neck, shoulder, or chest, especially on the ipsilateral side of the catheter? These complaints may mean it is more than the patient is able to tolerate, however treatment may help to improve those complaints. Immediate removal when there is a need for another CVAD insertion may not be the best option. The next catheter could easily produce a similar event on the other side, so the goal is usually to leave it in place. The patient should be treated for DVT with systemic anticoagulation for as long as the CVAD is needed and for 3 months after it is removed. Information about this is found in two INS Standards - Standard 52 CVAD Associated Thrombosis and Standard 44 VAD Removal. The medical references are two evidence based guidelines. You might want to find these and share with colleagues and appropriate committees in your facility. Both of these publications can be downloaded free of charge. Click below to get the full text. Kearon, C., Akl, E. A., Comerota, A. J., Prandoni, P., Bounameaux, H., Goldhaber, S. Z., . . . Dentali, F. (2012). Antithrombotic therapy for VTE disease: antithrombotic therapy and prevention of thrombosis: American College of Chest Physicians evidence-based clinical practice guidelines. CHEST Journal, 141(2_suppl), e419S-e494S. http://www.ncbi.nlm.nih.gov/pmc/articles/PMC3278049/pdf/112301.pdf Debourdeau, P., Farge, D., Beckers, M., Baglin, C., Bauersachs, R. M., Brenner, B., . . . Bounameaux, H. (2013). International clinical practice guidelines for the treatment and prophylaxis of thrombosis associated with central venous catheters in patients with cancer. J Thromb Haemost, 11(1), 71-80. doi:10.1111/jth.12071 http://onlinelibrary.wiley.com/doi/10.1111/jth.12071/epdf
Lia Kutzscher
6/13/2016 07:21:17 pm
Thank you Lynn for keeping me up-to-date and informed! Great opportunity for me to share with my malignant hematology team! Comments are closed.
|
Author: Lynn HadawayLynn Hadaway is an international thought leader in infusion therapy and vascular access, having been in this practice for more than 40 years. Her experience comes from hospital-based infusion teams, device manufacturers, and continuing education services. Her journal and textbook publications are extensive. She also maintains board certification in infusion nursing (CRNI) and nursing professional development (RN-BC). Categories
Archives
May 2019
|
Copyright © 2020 Lynn Hadaway Associates, Inc. | P.O. Box 10, Milner, GA 30257 | 770-358-7861


 RSS Feed
RSS Feed